Endometriosis
Endometriosis is a relatively common condition that may be associated with pelvic pain and difficulty conceiving. The lining of the womb is called the endometrium and endometriosis is defined as the presence of tissue outside the womb which is very similar to endometrium. The causes of endometriosis are poorly understood but it appears that this abnormal distribution of endometrium-like tissue causes inflammation and scarring which may then lead to symptoms. The course of endometriosis is difficult to predict as it may spontaneously regress in up to a third although in 50% the disease is progressive – worsening with time.
As with most benign conditions treatment depends on symptoms and the impact of those symptoms on quality of life.
Symptoms of endometriosis
Pelvic pain
Painful periods
Pain during intercourse
Subfertility (difficulty or delay in conceiving)
Bowel pain and rectal bleeding during menstruation
Abnormal vaginal bleeding
Heavy periods
Pain or bleeding passing urine
Diagnosis of endometriosis
Unfortunately many women with endometriosis see a number of doctors before the diagnosis is made and there is often a significant delay from first symptom to appropriate treatment. Equally some women are labelled as suffering from endometriosis when in fact other conditions related to bowel or bladder function are responsible for their symptoms. Unsurprisingly many women with pelvic pain spend years receiving the wrong treatment.
Any woman with symptoms suggestive of endometriosis should be asked a comprehensive series of questions by their doctor and an examination should also be performed. Usually a pelvic ultrasound would be organised to help identify other causes of pelvic pain and in particular to look for endometriosis in the ovaries where it can cause cysts called endometriomas. In some cases (particularly where severe disease is suspected) a more detailed MRI scan may be helpful.
Whilst symptoms, examination findings and imaging can all be helpful none of these techniques can definitively diagnose or exclude endometriosis. Currently the only sure way to make the diagnosis is to perform a laparoscopy (which is a surgical procedure using a small telescope which is placed through the belly button). The advantage of this approach is that it not only allows accurate assessment of the pelvis but also treatment at the same time. There are however risks with any surgical intervention and it may not be appropriate in all patients. In making decisions about invasive tests or treatment options the impact of symptoms on quality of life must be assessed first.
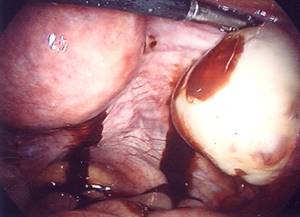
Endometrioma

Peritoneal Endometriosis
Conservative treatment
In women with mild symptoms it may not be necessary to treat endometriosis particularly as in up to 30% of cases the condition can spontaneously get better. Lifestyle measures such as increasing exercise and changing diet can be very important in managing endometriosis whilst simple painkillers may also reduce the symptoms. Alternative health techniques including dietary manipulation, acupuncture and reflexology may also be helpful and complement conventional medical treatments.
Medical Treatment of Endometriosis
As endometriosis is driven by the cyclical hormonal changes of the menstrual cycle all medical treatments involve hormonal manipulation to some degree.
Most hormonal treatments are equally effective at controlling endometriosis and so the actual treatment used should depend on the individual needs of the woman and the side-effect profile of the medicine.
Treatments could include:
Combined oral contraceptive pill
Progesterone only pill (‘mini-pill’)
Mirena coil (a progestagen releasing contraceptive coil)
Implanon (progestagen implant)
In addition a group of drugs called the GnRH analogues (eg zoladex, triptorelin, prostap) are often used in endometriosis. These drugs induce a temporary artificial menopause and are associated with side-effects including hot flushes and sweats and in the longer term – thinning of the bones. They should generally only used where other treatments have failed or prior to surgery for severe disease.
There are other drugs that have been used to treat endometriosis in the past such as danazol that are now rarely used due to their unacceptable side-effects.
It is also essential to offer appropriate pain relief which would normally include anti-inflammatory medications.
Surgical Treatment
Surgery for endometriosis is indicated when medical treatment has failed or is unacceptable or inappropriate. In women trying to conceive medical treatment is almost always inappropriate as the drugs are generally contraceptive and there is no evidence that after drug treatment fertility is improved. As a result all medical treatment does is delay trying to conceive.
In principle all women with known or suspected endometriosis and difficulty conceiving should be offered surgery which should be by laparoscopy. The available evidence suggests that treatment of endometriosis in this way improves fertility. This is especially true where there is an endometrioma (endometriosis of the ovary causing cyst formation). Surgical treatment of endometriosis prior to fertility treatments such as IVF is also often recommended.
There is also good evidence that surgical treatment of endometriosis reduces pain and improves quality of life. Even in the most severe cases of endometriosis the expectation should be that keyhole surgery can be performed to minimize the trauma of surgery and improve recovery. Keyhole surgery also allows a much better view of the pelvis compared to open surgery and more complete treatment of disease.
Rectovaginal endometriosis
A relatively small group of women have so-called rectovaginal (also known as Deep Pelvic Endometriosis) disease. In these
This kind of disease can also almost always be treated laparoscopically but is major surgery with significant implications. As with any
This kind of surgery should usually only be carried out by advanced laparoscopic surgeons with experience of this kind of endometriosis and would typically involve a multi-disciplinary approach with radiologists and colorectal (bowel) surgeons.
NICE guidance on endometriosis – https://www.nice.org.uk/guidance/NG73
Request an appointment
Clinics run three times a week, Gail or Anna will help you arrange an appointment to see Mr. Miskry.
If you are pregnant, you can expect to have a number of routine tests and appointments and you can find out more about the schedule of care here.
Appointments can be arranged by phone or email.
What our patients say about us
FAQs
These are some of our most commonly asked questions, but you can see all of them here
Do I need a GP referral for private treatment?
No. However if you have private medical insurance please check with your insurer as they may require a GP referral in order to provide cover.
Where does Mr Miskry see patients?
All clinics are held at 148 Harley Street.
Where does Mr Miskry perform operations?
The Lindo Wing, St Mary’s Hospital and King Edward VII’s Hospital.
If I have a private consultation will this alter my care in the NHS?
No. Your treatment or position on an NHS waiting list will not be affected by having had a private consultation/surgery.
Are tests included in my consultation fee?
Any tests Mr Miskry recommends as part of your care are payable directly to the clinic/lab/hospital where they are carried out and are not part of our fees.
